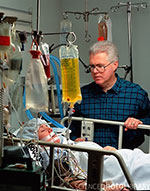
 We have all watched it unfold on soap operas, medical dramas and films: A patient falls into a coma, and loved ones at the bedside try to peel away the veil by talking or reading aloud. Some of us have done it ourselves, desperately hoping for any hint of wakening or awareness. For Theresa Louise-Bender Pape, who studies patients with traumatic brain injury (TBI) in various stages of coma and recovery, the “it can’t hurt” reasoning just is not good enough. She needs evidence. She wants answers. She is now testing two new therapies, familiar voices and magnetic stimulation, in two clinical trials.
We have all watched it unfold on soap operas, medical dramas and films: A patient falls into a coma, and loved ones at the bedside try to peel away the veil by talking or reading aloud. Some of us have done it ourselves, desperately hoping for any hint of wakening or awareness. For Theresa Louise-Bender Pape, who studies patients with traumatic brain injury (TBI) in various stages of coma and recovery, the “it can’t hurt” reasoning just is not good enough. She needs evidence. She wants answers. She is now testing two new therapies, familiar voices and magnetic stimulation, in two clinical trials.
Pape thinks and talks fast, and her hectic schedule keeps her on the go. The speech pathologist and neuroscientist travels regularly between Washington, D.C., because she works for the Department of Veterans Affairs, and Illinois, where she is based at the Hines VA hospital and is on faculty at Northwestern University’s Feinberg School of Medicine. Her nonstop pace makes it seem as if she is trying to make up for lost time, and, in a way, she is – but not for herself.
Pape has made it her life’s work to develop therapies that will, essentially, jump-start the lives of patients with traumatic brain injury. Her study subjects are veterans, warriors, and civilians who are in states of disordered consciousness (vegetative and/or minimally conscious), people who she says often fall silently through the cracks of the medical system, sometimes going from an acute-care hospital to a nursing home with no rehabilitation regimen at all.
Her multiple appointments and affiliations speak to the wide net she has cast as she pursues treatments that may one day engage key parts of the brain that control and maintain arousal and alertness, the parts that really make us come alive.
“I’m not someone who can sit still,” she says. “I’m going to be most engaged in my life the more challenges you give me. It’s just the nature of who I am.”
But what really fuels Pape’s afterburners is the hope that, the next time she sees one of her patients, he or she will be sitting up and talking to her, which has, indeed, happened before. You can get hooked on a payoff like that.
At 10:30 a.m. Wednesday in Room 101 of the Walter E. Washington Convention Center in D.C., Pape will describe her work during a 20-minute talk at the annual meeting of the American Association of Anatomists, which is being held in conjunction with the Experimental Biology 2011 conference. Her symposium will include a series of talks about traumatic brain injury.
Pape’s talk will cover the unique challenges and the triumphs her team has experienced over the past few years while conducting two innovative clinical trials: one that pipes familiar voices into the ears of unconscious patients and one that sends magnetic pulses into the neuronal centers of the brain. Both projects are funded, in part, by the U.S. Department of Veterans Affairs, Rehabilitation Research and Developmental Service.
One of the studies is a double-blind, randomized trial in which family members and loved ones of the patients play very important roles. First, baseline tests are conducted using functional MRI to see which parts of a patient’s brain are activated by familiar voices and unfamiliar voices telling short stories or what Pape admits are “rather lame jokes” and then nonverbal sounds, such as bells and whistles.
For the next six weeks, participants listen to digital recordings of their friends and relatives telling stories of escapades in which they and the patient participated. The therapy consists of four, 10-minute listening sessions each day, seven days a week for six weeks.
“We’ve had sisters tell stories from childhood like, ‘Remember when we had breakfast together and mom would make eggs and we’d hide them under our plates?’” Pape explains. “If it’s about a ski trip, we want adjectives so that the patient can envision motion and flying down the hill.”
The effect of the familiar voice intervention is determined with bedside tests of neurobehavioral functioning as well as fMRI and diffusion tensor imaging (DTI).
“Neurobehavioral functioning is a measure that reflects the level of each patient’s neural functioning from a behavioral perspective. The neurobehavioral or bedside measures will determine if neural functioning, measured behaviorally, is better after receiving the familiar voice intervention,” Pape says. “Both fMRI and DTI will be used to see if the mediators of neurobehavioral functioning can be identified.”
Pape has worked with 13 subjects so far, most of them male and about one-third of them veterans or warriors, and she intends to enroll up to 45 participants. About one-third of the patients are being cared for in nursing homes.
“I wanted to give families, therapists, and physicians a treatment that held promise, that could easily be done at the bedside, and be easily administered and relatively cheap to do,” Pape says. “It would be nice if everybody, regardless of if they’re in a nursing home or not, was getting to listen to familiar stories.”
In the second trial, Pape works with hospitalized patients who get around-the-clock care. She is investigating the safety and efficacy of transcranial magnetic stimulation (TMS). That is a fancy way of saying that she wants to know if it is safe and potentially helpful to place a special figure-of-eight-shaped coil on a patient’s scalp to transfer magnetic pulses, originating from a generator, into brain tissue, subsequently making neurons fire. Pape says she hopes that repeated stimulation will make the neurons “talk to each other.”
“Over time, I would love it if one neuron in the front relayed information to other neurons, ultimately transmitting this information to the brain stem and thereby reactivating those systems that maintain our arousal and alertness and then kicking back up to the thalamus and re-engaging our cortices,” she says.
So far, two patients have completed the noninvasive TMS therapy, which consists of 30 treatments. The first patient, over time, improved from a vegetative state to a minimally conscious state. The second improved from a vegetative state to a conscious state.
“At the end of 30 treatments, the second patient was minimally conscious. He wasn’t fully conscious yet, but he hadn’t received any rehab at all,” Pape says. So she helped arrange for him to get rehabilitative therapy at his nursing home, and he started receiving new medications. “He went six weeks without our experimental treatment, and, when we readmitted him, he was sitting up and he started talking to us!”
“Watching our patient suddenly start talking was really cool,” she adds.
After Pape’s talk, three presentations will be given by Peter Bergold of the State University of New York-Downstate Medical Center, Walter High of the University of Kentucky and the Lexington VA Medical Center, and Dorothy Kozlowski of DePaul University.
Material adapted from Federation of American Societies for Experimental Biology (FASEB).
No comments yet.